Labour pains: Why our growing maternity crisis is delivering agony nationwide
The maternity crisis gripping central Queensland also has interstate hospitals in its clutches, a national emergency that needs a combined federal and state government response, according to the Rural Doctors Association of Australia (RDAA).

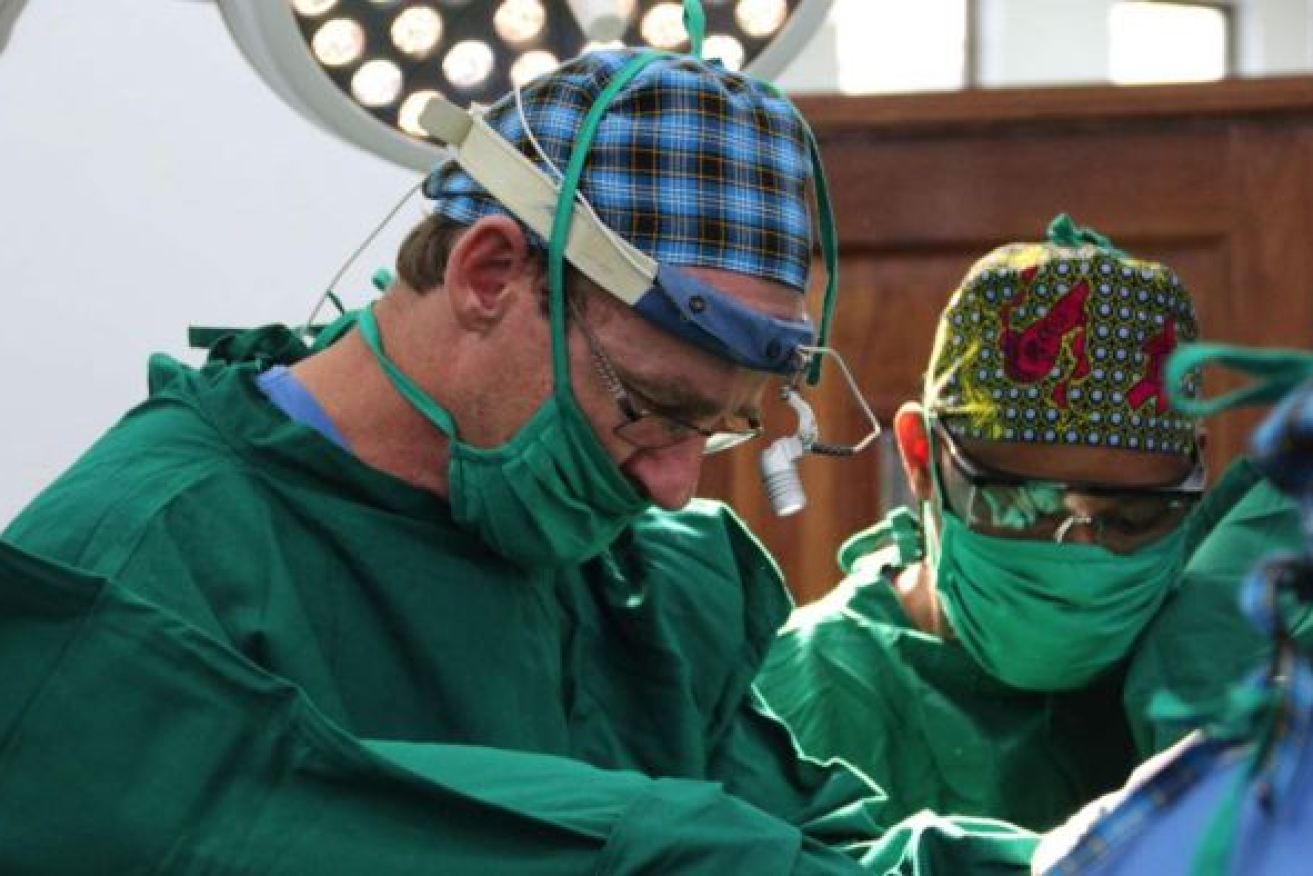
Rural doctors say they are being nudged away from involvement in maternity cases. Photo: ABC
As birthing units at Gladstone and Biloela remain on bypass, the RDAA has revealed that more hospitals beyond the central Queensland region are under similar stress.
With heavy rain and flooding throughout the region hampering travel and stretching emergency services, grave concerns are now held that pressure will continue to build on an already strained Rockhampton Hospital to accept more pregnant women who can no longer access the smaller centres.
The bypass is preventing most local women from giving birth in the hospitals, unless by elective caesarean, and they instead have to drive more than 100km to Rockhampton when they go into labour.
Beaudesert Hospital in the state’s south east, one of the few maternity units to have been revived in recent years following mass closures of rural birthing units in the early 2000s, has been on obstetric bypass several times in the last month, according to the RDAA.
The disruption to maternity services at what was once one of Queensland’s busiest rural maternity units, will come as a bitter blow to health professionals and medical administrators.
Reopened during the term of the Newman LNP Government under then Health Minister Lawrence Springborg, the reopened Beaudesert Hospital was often cited as a best practice model for rural communities fighting to have their maternity services restored.
Pregnant women in Ingham and Cooktown benefited from the Beaudesert experience.
But according to a recent statement from Rural Doctors Association of Queensland president Dr Matt Masel, those centres also remain vulnerable.
“More recently we have doubled efforts as units like Chinchilla and Weipa struggle to get the required workforce to reopen,” Masel said.
“And, now with larger units such as Gladstone on bypass, what has been a long-term rural challenge has now become a regional one as well.
“In reality that means multiple trips far from home for expectant mothers, time away from work and family and risks of roadside birthing, and worse.”
The deepening crisis has led to calls from Opposition Leader David Crisafulli for Health Minister Yvette D’Ath to resign.
D’Ath told reporters on Wednesday that it would be unsafe to restart full birthing services at Gladstone until all 10 obstetrician positions were filled at the Central Queensland Hospital and Health Service.
“What would be unacceptable is if we sought to bring those services back online in an unsafe way, we cannot do that,” she said.
“I have to take the advice as the minister in ensuring that these services are reintroduced in a safe way. I’m being told that we need 10 FTEs, full-time equivalents, across Rockhampton and Gladstone.”
But the challenges are not only confined to Queensland, with the city of Geelong near Melbourne, also facing the prospect that a private facility, Epworth Healthcare, will shut its maternity unit in March.
The acute shortage of midwives, specialist obstetricians and rural generalist doctors with advanced obstetric skills, has been blamed for the closures.
RDAA president Dr Megan Belot said an “extensive number” of regional and rural locations across Australia, as well as centres in major regional cities like Geelong, had long-standing vacancies for staff required for safe birthing.
“Enough is enough,” she said
“In a wealthy country like Australia, we should be able to guarantee that when a woman needs to go to hospital to give birth – either for a planned delivery or an emergency delivery – she should be able to access the care she needs.
“Unfortunately, this is clearly not the case, and these recent examples are sadly the tip of the iceberg when it comes to the continuing erosion of regional and rural birthing services across Australia.”
D’Ath said she welcomed the government’s efforts to help Queensland Health and Central Queensland Hospital and Health Service to bring obstetric services online as quickly as possible, but cautioned the solution was “not about dollars”.
“You know if it was that simple, you know, we would have the obstetricians there. It is about a lack of obstetricians nationally right now, and particular challenges at that hospital due to personal circumstances and a range of reasons why other obstetricians who were there had to move on,” she said.
Both Belot and Masel continue to advocate for increased funding for rural generalist training, allowing doctors based in rural locations to operate over a wider scope of practice.
As previously reported by InQueensland, the rural generalist model was first developed and championed by Queensland doctors before it was boosted with federal funding from the former Morrison government as the National Rural Generalist Pathway (NRGP).
However, Belot maintains the NRGP has been only “half implemented”.
“We are hopeful that, in light of the latest planned closure and bypasses, the federal and state governments will work urgently to get the pathway fully up and running across the country,” she said.
“Until we start to get real about training more rural generalist doctors with advanced skills in obstetrics and other areas, expose more junior doctors to rural medical careers by boosting the number of rural training places available, and implement better pathways to expand the rural nursing and midwifery workforce, the future of rural maternity care will remain extremely fragile.
“And those at greatest risk will be rural women and their babies.”












