Qld’s last virus death was 335 days ago – yesterday five people died on our doorstep
While the official figures are bad, the real toll of the COVID-19 outbreak in Papua New Guinea is probably much, much worse. As Sean Parnell writes, the country’s medical history is alarming.

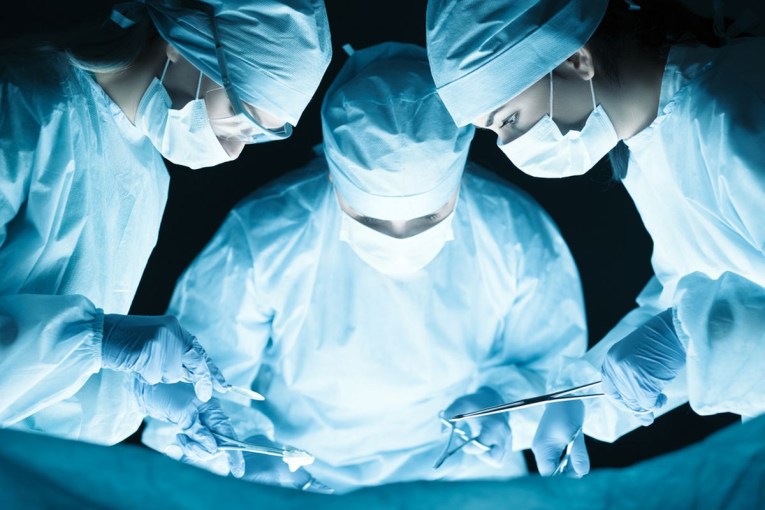
Tents are being set up as emergency testing stations in the carpark of PNG's biggest hospital (ABC image)
The Torres Strait is not some far away, magical place, although it is magical. It is only slightly further away from Brisbane than Melbourne is in the other direction. But once you get past Cape York, Papua New Guinea looms large, and can be seen from some islands: this is Australia’s nearest, but often overlooked, neighbour, where tradition enables close relations between communities that share the benefits, and challenges, of splendid isolation.
For many Australians, the Torres Strait is out of sight, out of mind, yet the latest PNG health crisis is something that has been hidden in plain sight for years. The PNG health system has long struggled to respond to the needs of its impoverished population, and while Australia can afford to spend money promoting positive health behaviours, and propping up private health, to the north they struggle with infectious diseases such as HIV, multi-drug resistant tuberculosis and malaria. Health workers are dedicated but up against it; it’s no surprise PNG nationals die, on average, almost two decades before Australians.
Now, the pandemic has hit – hard. COVID-19 cases have soared over the past month, with Papua New Guinea now recording more new cases in a day than Australia records in a week – and most of unknown origin. But everyone knows it is already much worse than that.
As Prime Minister Scott Morrison bluntly put it this week, Australia has been monitoring COVID-19 in the region “but we’ve known that that challenge was always going to be too great for Papua New Guinea as time went on”. It probably didn’t help that PNG’s other neighbour, Indonesia, downplayed the spread of COVID-19 for so long.
The five deaths reported in PNG yesterday, and 36 overall, are likely to dramatically underestimate the scale of the problem, something Australia’s Deputy Chief Health Officer Paul Kelly has acknowledged. The closest thing to population screening, tests on pregnant women in Port Moresby and workers at the Ok Tedi mine, have revealed roughly a 50 per cent infection rate.
People are sick, and dying, with their carers sometimes not realising they have also been infected. COVID-19 has spread rapidly among health workers. The probable number of cases, in a population of 8.8 million, is unfathomable.
Australia is now sending 8,000 doses of COVID-19 vaccines to help protect PNG health workers, and will soon dispatch a medical team to provide support on the ground. This is different territory: Australia might have the anti-vaxxers of Mullumbimby and the odd rogue backbencher or fragile celebrity chef to deal with, but in remote parts of PNG some people still believe in witches. There has been little compliance with, or enforcement of, public health measures, and official health department text messages start by telling people “COVID-19 is real”.
Yet allowing the uncontrolled spread of COVID-19, even bungling vaccination and treatment, could create new variants that pose an even greater risk, not only to PNG but the region. That has happened before with TB.
Recognising the threat, Queensland Health had already diverted COVID-19 vaccines to the Torres Strait, hoping to be able to protect communities before the virus arrives. Around 159 people have already had their first shot, as clinicians work their way back from the PNG border to eventually vaccinate Cape York communities too.
In an extraordinary move, arrangements are being made for some Queensland Health workers to cross the border and start vaccinating nearby PNG communities too. They hope to be quick enough to build a buffer zone.
Early in the pandemic, travel to remote Aboriginal communities on Cape York was restricted to keep the virus out, given residents have health conditions that put them at greater risk and health services are limited. The same has happened in the Torres Strait, where cross-border travel between certain villages is normally allowed. Now, even flights from PNG are being restricted.
Premier Annastacia Palaszczuk was in far north Queensland this week and found people worried about COVID-19 coming from PNG. Overnight, even after the restrictions were imposed, another six travellers from PNG tested positive in hotel quarantine, of nine extra cases overall.
The Commonwealth is increasing surveillance in the Torres Strait. A tinnie with an outboard motor could make it from PNG to Australia faster than well heeled Sydney-siders could do a sunset cruise of the harbour.
If COVID-19 were to spread through the Torres Strait, Australia’s world-class health system and envied response to the pandemic would suddenly appear fallible. Expect aero-medical retrievals from Thursday Island to Cairns, where COVID-19 patients – returned travellers from PNG diagnosed in hotel quarantine – are already having to be flown on to Brisbane to free up beds.
Palaszczuk has already warned about the cracks in hotel quarantine. Today, she warned of a time when Queensland hospitals may no longer be able to take infected travellers.
“There may come a time where that is going to prove difficult,” the Premier said.
“We’re seeing nine, eight a day. We’ve just got to see how our hospitals go at the moment and we’re just going to have to look at contingency plans.”
Over the years, this added burden on Queensland Health from PNG has become a source of friction between the state and federal governments. Queensland has often had to go cap in hand to Canberra to ask for more funds to treat patients and new arrivals. There is a tacit acknowledgement that the better the health services are in the Torres Strait, the more likely desperate PNG nationals are to make the trek across the border, so more work needs to be done on the other side.
Yet relations between Australia and PNG are sometimes strained too, particularly when corruption and mismanagement has undermined previous health investment. Progress is slow, sometimes fatally slow, and people are dying needlessly on Australia’s doorstep.
In 2010, Australia finally managed to reach agreement with PNG to upgrade water infrastructure on Daru, one of the closest PNG islands to the Torres Strait. It took a cholera outbreak to seal the deal, and by then dozens of people had died of a preventable infection more often seen in third world countries.
For the people of PNG, and communities in the Torres Strait, let’s hope help doesn’t arrive too late this time.